Patient journey:
Follow these steps to a better quality of life
Phase 1: Self-management
When should I see a general practitioner?When should I see a general practitioner?
- You are still unable to control your sinusitis symptoms despite lifestyle changes and nasal rinsing
- If your symptoms are unilateral (on one side of the body/nose) and lasting for more than 4 weeks
- You think you have another condition that strongly resembles the symptoms of chronic sinusitis
- You are looking for a diagnosis and treatment by a physician (depending on your countries medical system you may also be able to see an ear-nose-throat (ENT) doctor without prior consultation with a general practitioner (GP) if phase 1 is insufficient)
Phase 2: General Practitioner
When should I see a specialist?When should I see a specialist?
- You are still unable to control your symptoms despite first-line treatment with nasal rinsing and nasal corticosteroids and a consultation by a general practitioner (GP)
- You need further diagnostic testing that can only be performed by an ear-nose-throat doctor (ENT)
What is chronic sinusitis?
Sinusitis refers to inflammation of the mucous membrane in the nasal cavity and paranasal sinuses, and is accompanied by:
- Facial pain or pressure
- Disrupted sense of smell
- Runny nose
- Blocked nose
- Mucus leaking down the throat
When two or more of these symptoms (of which certainly a runny or blocked nose) continue for more than 12 weeks without a break, we call this chronic sinusitis. Some patients might also experience ear or teeth pain, bad breath, sore throat, irritability and lack of energy.
The complaints associated with chronic sinusitis can have a major impact on a patient’s daily life. Fatigue and disrupted sleep are common, which mean you have less energy to carry out daily activities in the normal way. In some cases this can affect a person’s performance or cause absence from work.
Do you suffer from chronic sinusitis?
Then you are not alone. About 10% of Europe’s population suffers from this problem. The development of chronic sinusitis is often due to a combination of the following factors: environment (pollution or exposure to irritants), lifestyle (smoking or low immunity), hormones and genes.
There are various forms of chronic sinusitis: with or without nasal polyps. Furthermore, an affliction in the upper airways (nose and paranasal sinuses) can affect the performance of the lower airways (lungs). If you have sinusitis, you can therefore also develop asthma. Do visit your doctor if you have any complaints. The doctor can confirm whether or not you have asthma.
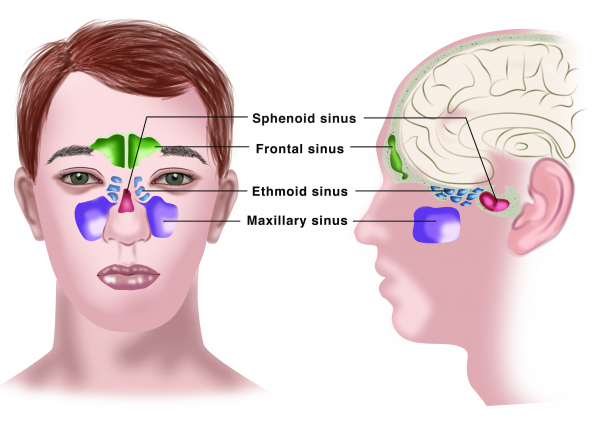
What are sinuses?
Sinuses are cavities in the skull next to and in connection with the nasal cavity. In healthy individuals, sinus cavities are covered with mucosa and filled with air. The nose and sinuses are important for filtering, heating and moistening the air you breathe in through your nose, which is important for optimal lung function. Sinus cavities may also contribute to voice resonance and can absorb energy to protect the
brain from trauma.
What are nasal polyps?
Chronic (rhino)sinusitis can present with nasal polyps (CRSwNP) or without (CRSsNP). Nasal polyps are grape-like mucosal outgrowths with inflammation inside, and often cause smell impairment, headache and/or nasal obstruction. Unlike intestinal polyps, sinonasal polyps that are found in both cavities of patients with (rhino)sinusitis do not turn into malignant disease.
COVID-19
I have chronic rhinosinusitis. Am I at risk to get more severe COVID-19 symptoms?
According to existing evidence, COVID-19 does not appear more severe in patients with chronic rhinosinusitis (CRS). CRS is often accompanied by lower airway symptoms – even if no asthma has been previously diagnosed. In general, be vigilant on COVID-19 symptoms (e.g. loss of smell, ‘’common’’ cold or flu-like symptoms, fever and lower airway symptoms: cough, shortness of breath). It is important to keep your CRS well-controlled and to follow the treatment advice of your physician.
Is there a difference in the mechanisms driving loss of smell in chronic rhinosinusitis and SARS-CoV2 infection (the virus causing COVID-19)?
The loss of smell (anosmia) in chronic rhinosinusitis (CRS) (often in combination with nasal polyps) is caused by chronic inflammation of the nasal and sinus mucosa. In COVID-19, the exact mechanism of potential olfactory nerve damage in the nose is not fully clear. If your loss of smell is caused by COVID-19 infection, it may subside in a few weeks or months after recovery. If you experience a loss of smell during the COVID-19 pandemic, do not hesitate to contact your physician.
Causes and symptoms
Frequently Asked Questions
Acute or chronic (rhino)sinusitis?
Inflammation of the mucosa of the paranasal sinus cavities can be split into 3 categories: common cold, acute (less than 12 weeks of time) and chronic (over 12 weeks of duration) (rhino)sinusitis. Common cold is a self-limited disease, often of viral origin, lasting for 1 to 2 weeks, and with gradual resolution of symptoms with or without treatment. Acute (rhino)sinusitis is defined as sinus disease lasting up to 12 weeks. (Rhino)sinusitis is considered to be chronic when symptoms last for 12 weeks or longer. Chronic (rhino)sinusitis might present with stable symptoms or be subject to disease exacerbations.
Why do I have smell impairment?
When you smell something, inhaled particles reach the upper part of the nose and bind with the receptor cells on the smell organ, called olfactory organ, which is located high in the nasal cavity. Chronic (rhino)sinusitis, especially with nasal polyps causes inflammation in or around the olfactory (smell) mucosa, leading to a reduced sense of smell or even smell loss. In addition to local inflammation of the olfactory organ, polyps might impair the arrival of inhaled particles to reach the olfactory organ. Current treatment for chronic rhinosinusitis aims at restoring smell impairment by either reducing the inflammation in and around the olfactory organ, or by removal of the nasal polyps by medical or surgical treatment.
Does chronic (rhino)sinusitis progress when I get older?
Chronic (rhino)sinusitis is different in children compared to adults, with less polyps in children unless they suffer from cystic fibrosis. There is some evidence that chronic (rhino)sinusitis changes its type of inflammation with ageing. Chronic (rhino)sinusitis with nasal polyps becomes more severe with time when left untreated. Moreover, polyps growing over time may exert pressure on the bone even causing deformities of the midface. Another sign of disease progression is the onset of asthma symptoms such as shortness of breath, wheezing, coughing and sputum.
What are the differences between a prolonged cold and chronic (rhino)sinusitis?
A common cold is often viral in origin, and self-limiting. Many patients with chronic (rhino)sinusitis remember an infection of the nose as the first event of their chronic illness. This infection might have triggered the development of rhinosinusitis, or might be the consequence of an existing inflammation with aggravation by the infectious agent. Chronic rhinosinusitis is defined as a persistence of symptoms of the nose and sinuses for more than 12 weeks. The role of viruses and bacteria in chronic rhinosinusitis is not clear.
Can chronic (rhino)sinusitis be cured?
In general, rhinosinusitis is a chronic disease with a wide spectrum of disease severity and presentation patterns. Patients might have long periods of well-controlled disease, or experience gradually increasing or stable disease. The treatment aims primarily to control patient's symptoms. Other goals are to reduce mucosal inflammation, to facilitate the drainage of secretions from the sinus cavities to the nose and to reduce sudden worsening of symptoms. Usually the disease becomes less severe in the elderly.
Are my headaches caused by chronic (rhino)sinusitis?
Headaches can be caused by chronic (rhino)sinusitis, especially in association with other symptoms like nasal obstruction, smell impairment, runny nose and/or secretions dripping into the throat. The headache is usually located around the eyes, in the forehead or in the cheek area, and is usually described as a dull pressing feeling. Pain located at the side of the head or in the neck is seldom caused by chronic (rhino)sinusitis.
Is chronic (rhino)sinusitis caused by my allergy?
Allergy is not the cause of chronic rhinosinusitis, but might worsen the inflammation of the mucosa in patients with chronic rhinosinusitis. Any neglect of allergy as concomitant factor causing or aggravating sinonasal symptoms might lead to a dissatisfied patient.
If patients with rhinosinusitis and pollen allergy experience more nasal symptoms during the pollen season, it makes sense to adequately diagnose and treat the allergy component. If patients are sensitised to moulds, animal dander or house dust mites, it makes sense to undertake the proper measures to reduce exposure and to treat the allergic component of rhinosinusitis according to the symptom severity and control of disease.
What is the link between chronic (rhino)sinusitis and asthma?
The upper (nose and sinuses) and lower (lungs) airways are closely related to each other. Good function of the nose and sinuses is important for the optimal function of the bronchi and oxygen handling in the lungs. Up to one third of patients with rhinosinusitis have bronchial symptoms, like asthma and chronic bronchitis. Most patients with asthma have inflammation in the nose (rhinitis), with one third having rhinosinusitis. The presence of inflammation and symptoms at both ends of the airways, i.e. upper and lower airways, should be considered at the time of diagnosis and design of the therapeutic plan.
What is the link between nasal polyps, asthma and respiratory reactions to aspirin?
Aspirin-exacerbated respiratory disease (AERD), also called Samter's triad, is a chronic condition that consists of three clinical features: asthma, nasal polyps, and respiratory reactions to aspirin. About 9% of all adults with asthma and about 30% of adults with both asthma and nasal polyps have AERD. The clinical diagnosis of AERD can be made if all three of these features are present. The exact cause of AERD is unknown. There is no evidence to suggest that it is genetic or inherited. The disease is not caused by taking aspirin or other non-steroidal anti-inflammatory drugs (NSAIDs), but sinus or asthma symptoms can worsen when taking these medications.
Is chronic (rhino)sinusitis inherited?
Chronic (rhino)sinusitis with or without nasal polyps are mostly seen without a suspicion of a hereditary (genetic) factor. Specific forms of chronic rhinosinusitis might have a genetic predisposition, with the disease running in families. Studies in genetically identical twins showed that both siblings will not necessarily develop nasal polyps, which emphasizes the role of non-hereditary environmental factors.

Which lifestyle changes can help?
Lifestyle factors like smoking, work-related or environmental exposure to certain agents (or irritants) and air pollution may affect chronic (rhino)sinusitis. It is generally accepted that these lifestyle factors might contribute to the development and/or chronic nature of the disease and should be considered in those patients with difficult-to-control rhinosinusitis.
The role of gastric acid reflux, nutrition and microbiological flora in rhinosinusitis is still under exploration and hence a matter of debate.
Lifestyle changes
Frequently Asked Questions
How much does smoking influence my nasal problems?
Inhaled pollutants like cigarette smoke are major causes of irritation to the airways, and it hinders clearance of mucus from nose and sinuses. Cigarette smoke, either active smoking or passive exposure, contributes to the development of chronic (rhino)sinusitis. Smoking induces mucosal swelling in the nose, increases the likelihood of airway infections and reduces the sense of smell. Active smoking is not a reason not to perform sinus surgery.
Why do I need to stop smoking? I have been smoking for years but my chronic (rhino)sinusitis just started recently.
Smoking is a major factor causing irritation in the bronchi and lungs, but also in the nose and sinuses. Smoking-induced irritation can be more severe in patients with chronic (rhino)sinusitis than in healthy individuals. Smoking cessation is recommended in rhinosinusitis as it may be associated with reduced inflammation and burden of disease. It is however difficult to predict the impact of smoking cessation on the inflammation and burden of (rhino)sinusitis in an individual patient.
When I drink alcohol, I have more symptoms. I think that I am allergic to it. Is that possible?
Alcohol intolerance is seen in most patients with chronic (rhino)sinusitis, especially in those with rhinosinusitis with nasal polyps. Drinking of alcohol-containing liquids might cause congestion of the nose and sinuses, and aggravate disease severity. The mechanisms giving rise to alcohol-induced airways symptoms are not related to a classic allergic reaction, but rather associated with the activation of nerves in the sinonasal mucosa. Many patients with chronic rhinosinusitis refrain from drinking alcohol-containing liquids.
I think my chronic (rhino)sinusitis started when I inhaled some water/chemical/gas/smell via my nose at work. Is that possible?
Irritation of the nose by chemical substances, gas or contact with contaminated water, can trigger an inflammatory reaction inside the nose and sinuses. One or repeated contacts with these agents might lead to longstanding mucosal inflammation and induction of symptoms. Chronic (rhino)sinusitis is usually caused by a combination of different factors. Other factors that you might not be aware of may have contributed to the development of your chronic (rhino)sinusitis.
I was very healthy until I worked at a place with poor indoor air quality. Afterwards I got the diagnosis of chronic (rhino)sinusitis. Did that cause my disease?
Poor indoor air quality and allergies to moulds and dust mites might cause inflammation and swelling inside the nose and sinuses in predisposed individuals, leading to chronic rhinosinusitis with/without nasal polyps. It is, however, difficult to conclude that these factors have caused the rhinosinusitis, as most patients have multiple reasons why rhinosinusitis develops at a certain time point in their life.

What can the pharmacist do?
Nasal rinsing with saline is considered a first-line treatment for chronic (rhino)sinusitis. It provides some symptomatic relief by washing the nasal cavities, removing secretions, reducing secretions dripping into the throat and rinsing away allergens and irritants that are contributing to the disease. Moreover, the use of nasal rinsing with saline prior to administration of other nasal medications enables the medication to effectively reach the inner lining of the mucosa of the nose.
Watch here instructional videos on how to use nasal sprays correctly and how to perform nasal rinsing.
Other over the counter (OTC) medicines are decongestant sprays or sprays with corticosteroids. The availability of nasal sprays with corticosteroids is country dependent. Ask your pharmacist which medication without prescription can be used for treatment of chronic sinusitis in your country. We recommend you visit a physician to have proper diagnostic testing if your symptoms are too bothersome.
Pharmacy
Frequently Asked Questions
What can I expect from the pharmacist?
Pharmacists are members of the multidisciplinary team that offer meaningful advice for treating chronic (rhino)sinusitis. They have knowledge about different drugs and can give useful advices on how to use nasal sprays. Some pharmacists can also advice you on how to perform nasal rinsing with salt water. The pharmacist will also stress the fact that a consequent use of nasal sprays with corticosteroids is essential to achieve the maximal benefit from this drug.
Additionally, counselling about the temporal effects of nasal sprays with corticosteroids can also be given by the pharmacist. Patients should know that it might take some days before they start to notice the beneficial effects of nasal sprays with corticosteroids and that the effect is not instantly like for example with decongestive sprays. However, to make a proper diagnosis and to get the follow-up needed, you must also see a doctor.
Why is nasal rinsing with saline necessary?
Nasal rinsing with saline is considered a first-line treatment for chronic (rhino)sinusitis. It provides some symptomatic relief by washing the nasal cavities, removing secretions, reducing secretions dripping into the throat and rinsing away allergens and irritants that are contributing to the disease. Moreover, the use of nasal rinsing with saline prior to administration of other nasal medications enables the medication to effectively reach the inner lining of the mucosa of the nose.
The nasal decongestant spray that I buy without prescription is much better in opening up my blocked nose. Why can I not use it all the time?
The nasal decongestant spray only works for a short period by decongesting the mucosa in a potent way. It should not be used longer than 7 consecutive days. If used over a longer period, it can have adverse effects like additional swelling and irritation of the mucosa and even cause addiction to this medicine.

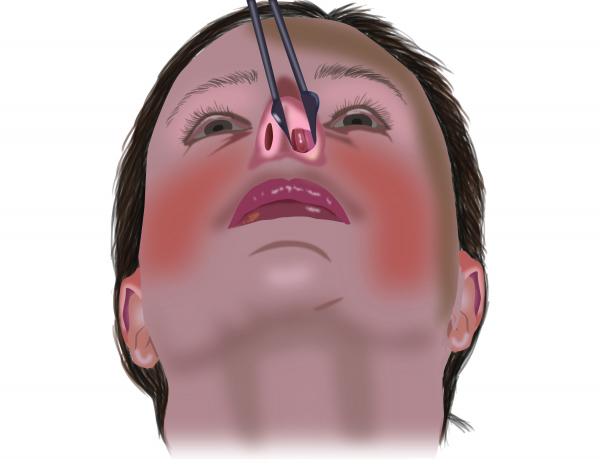
How is the diagnosis made?
In order to reach the correct diagnosis, your doctor will first discuss your symptoms extensively with you. He/she will carry out a physical examination to study the inside of your nose (which is called an anterior rhinoscopy). This examination can evaluate the condition of the nasal mucosa and detect the presence of larger nasal polyps. The presence of nasal polyps into the nasal cavity can lead to referral to an ear-nose-throat specialist.
Some general practitioners will perform skin prick tests when nasal allergies are suspected, depending on the availability of this test in their practice. A CT scan might also be ordered to help confirm a sinusitis diagnosis.
Diagnosis
Frequently Asked Questions
When should a patient with sinus symptoms seek medical advice from the primary care physician?
A "common cold" is considered self-limiting and symptoms should resolve within two weeks. The inflammation in common cold affects both nasal as well as sinus mucosa. Symptomatic treatment or pain killers might help. Medical advice is warranted in case of severe symptoms or clinical signs of complications, like swelling of the skin and tissues overlying the sinus cavities, problems with the globe or vision, or high fever. If a common cold persists beyond 2 weeks, the term acute rhinosinusitis is used, and patients are recommended to seek medical advice to get cured. In addition, a proper diagnosis including nasal endoscopy is warranted in case of symptoms at one side of the nose/face, nose bleeds and/or severe headaches.
How do I find a doctor to treat my sinusitis problems?
This depends on the health care system in the country where you live. In most parts of Europe, you should first seek help from your pharmacist and general practitioner. You may be referred to an Ear, Nose and Throat (ENT) doctor if standard treatment does not work. Standard treatment consists of nasal rinsing with salt water and nasal spray with corticosteroids.
What are the clinical signs of chronic (rhino)sinusitis?
When looking into the nose with an instrument called nasal speculum or endoscope, the doctor may find the sinonasal mucosa to be swollen, with or without the presence of polyps, and the presence of transparent or discoloured secretions. In most patients with rhinosinusitis, nasal examination with a speculum or endoscope suffices to make a proper diagnosis. In case of lack of availability of nasal endoscope, a CT scan can be considered.
How can chronic sinusitis be treated?
The main focus in the treatment of chronic sinusitis lies on controlling the symptoms. Further treatment can also reduce the inflammation of your mucous membranes and ease the drainage of mucus from the sinuses to the nose. The first step involves rinsing the nose with salt water. In doing so, you wash out the nasal cavity and paranasal sinuses and loosen the mucus that would otherwise drip into the throat.
After this procedure, nose sprays containing corticosteroids are more effective in reaching the inflamed mucous membranes. A nasal decongestant spray might be prescribed and can lead to instant relief of nasal blockage. If a general practitioner prescribes this spray, a follow-up should be scheduled, and the decongestant should be discontinued after 7 consecutive days.
COVID-19
Is treatment with corticosteroid nasal spray recommended for patients with COVID-19 who present with loss of smell?
Presently, there is no evidence that the use of a corticosteroid nasal spray leads to an increased risk of COVID-19 infection or trigger a more severe course of COVID-19. A considerable percentage of COVID-19 patients experience loss of smell as an early sign of the disease. There is no indication that intranasal corticosteroid treatment has a positive impact on the recovery. However, there is no evidence either suggesting that this treatment has a negative impact on the symptoms and/or the development of (more severe) COVID-19. Therefore, it is recommended to continue regular treatment with your corticosteroid nasal spray for chronic rhinosinusitis.
I take tablets with corticosteroids. Should I continue my treatment during the COVID-19 pandemic?
Chronic use of tablets with corticosteroids should be avoided or used with caution in patients with chronic rhinosinusitis (CRS) during the pandemic and should only be reserved for patients with severe symptoms and in the absence of an alternative. Treatment decisions (corticosteroids, surgery or biologics) should be taken on an individual basis. In case of worsening of your CRS symptoms, contact your physician, as starting or stopping corticosteroids on yourself may induce general health risks as well as may affect your CRS control. It may also affect your susceptibility to SARS-CoV2 infection (the virus causing COVID-19).
Treatment
Frequently Asked Questions
How do intranasal steroids work?
Intranasal (cortico)steroids are an effective drug in controlling the symptoms of allergic rhinitis, especially effective on nasal obstruction. The main mechanism by which intranasal steroids relieve symptoms is through their anti-inflammatory activity. They are effective in controlling the four major symptoms of allergic rhinitis: nasal congestion, rhinorrhoea, itching and sneezing. Nasal corticosteroid sprays also have a positive effect on the eye symptoms.
The effect of the intranasal spray starts after several hours, with maximal efficacy reached after several weeks of usage. Intranasal steroid sprays are safe for long-term use if patients follow the recommended doses and right application. The steroids are not taken up in the bloodstream and are therefore not associated with systemic side effects. Adverse reactions usually are limited to epistaxis (nosebleeds) due to improper application, nasal dryness/ crusting, abnormal taste and throat irritation.
What can I expect from medical treatment?
Medical therapy aims to reduce the burden of the disease in patients, with reduction of symptom severity and improvement of quality of life. When medical treatment is effective, patients might live a normal life without headache, and with normal nasal breathing, less secretions in the nose, and good smell capacity. Unfortunately, medical treatment does not often "cure" patients with chronic (rhino)sinusitis, as many remain having symptoms despite medical treatment. In some patients with severe symptoms despite medical treatment, surgery to open the sinus cavities and remove diseased mucosa is recommended.
What to do after a doctor visit?
Several treatments such as corticosteroids should be taken on a regular basis and only work after several weeks of treatment. It is important to adhere to the therapy that your doctor has prescribed you and to monitor your symptoms in between consultations. The long-term use of topical steroids is safe.
If your symptoms remain bothersome or if you develop new symptoms, it is important to take a new appointment with your doctor. If you have tried all first line treatments and remain uncontrolled, you might consider taking an/another appointment with an ear-nose-throat specialist. In case you also experience symptoms of the lower airways such as shortness of breath, it might be asthma and you should consider making an appointment with a pulmonologist.
Follow-up
Frequently Asked Questions
Why is it important to diagnose asthma in a patient with chronic (rhino)sinusitis?
Given the fact that bronchial symptoms are present in up to one third of patients with rhinosinusitis, it is important to recognise bronchial symptoms like cough, shortness of breath and wheezing in adolescents and adults with chronic sinonasal symptoms. Asthma can be diagnosed by a physician. In case asthma is present, it is important to treat the bronchial inflammation of asthma, as optimal condition of the bronchi will have a positive effect on rhinosinusitis. Treatment of chronic (rhino)sinusitis might be more difficult if asthma co-exists and combined therapy needs to be applied and adapted for both conditions.
When should I go to the specialist to receive a treatment for my sinus symptoms?
A patient should seek advice from a specialist (Ear, Nose and Throat doctor) when sinonasal symptoms are severe, not well controlled by the treatment by the general practitioner, and when measures to self-manage the condition fail. Urgent referrals are recommended in case of sudden onset of unilateral or severe disease, sudden onset of swelling of tissues over the sinus cavities or associated vision loss. In case of gradual unilateral nose or sinus problems lasting for more than 4 weeks, a physician should be consulted.

How is the diagnosis made?
Once the typical signs of sinusitis have been established, your doctor can also conduct an anterior rhinoscopy. This involves examining the foremost part of the nasal cavity. Should this examination remain inconclusive, the ear, nose and throat specialist will conduct a nose endoscopy. In doing so he/she will investigate your nasal cavity and paranasal sinuses using a narrow camera.
If an endoscopy is impossible, or if there is a difference between the clinical symptoms and the results of the endoscopy, your doctor will request a CT scan of the sinuses. This provides a detailed anatomy of the sinuses. In this way, the specialist can still track down an infection that failed to show up under the endoscope. In some cases, the doctor will perform additional blood tests to rule out other diseases that have symptoms resembling those of chronic sinusitis.

When and why is a CT scan advised?
A CT (computed tomography) scan is advised in case of chronic (rhino)sinusitis with or without nasal polyps before surgery, or when the ear-nose-throat (ENT) doctor considers confirmation of clinical suspicion by CT scan necessary. The CT scan will not only show the severity and extent of disease and its relationships with other surrounding structures but will also work as a map for the ENT doctor, showing important anatomical landmarks during surgery.
In summary, this information helps in making a diagnosis and in case of surgery it helps the ENT doctor during the sinus surgery.

How can loss of smell be tested?
Smell can be tested in a subjective way by means of different smell tests such as UPSIT (University of Pennsylvania Smell Identification Test), Sniffin' Sticks, Barcelona smell test or other available screening tests. Additionally, there is a way to do an objective measurement by means of smell evoked current measurements. In specific cases of severe or unexplained smell loss, an MRI scan of the olfactory bulbs (smell region in the brain) is warranted.
Diagnosis
Frequently Asked Questions
Which tests are usually done to diagnose my chronic (rhino)sinusitis?
Several technical examination methods are available to determine nasal patency. They include rhinomanometry (measuring pressure and flow during normal inspiration and expiration through the nose), acoustic rhinometry (determining the structure of the inside of the nose by transmitting sound waves through the nose) and peak nasal inspiratory flow (measuring nasal flow during forced inspiration through the nose) measurements and can be of use to objectify reported nasal blockage and measure nasal airflow. When nasal endoscopy is not available or when there is discrepancy between clinical symptoms and endoscopy, a CT scan of the sinuses might be performed. Smell tests can be required to determine a possible loss of smell and skin prick tests may be performed for diagnosing allergy to inhalant allergens like dust mites or pollen.
What is the role of nasal endoscopy in the diagnosis?
Nasal endoscopy is indispensable in the diagnosis of chronic (rhino)sinusitis. It offers the advantage of a global evaluation of the nasal cavity and the outflow tracts of the sinuses visualizing the oedema of mucosa, presence of nasal polyps and/or secretions. In case nasal endoscopy is not feasible or possible, a CT scan of the sinuses is recommended to diagnose chronic rhinosinusitis. Other tests might be performed upon specific indication or symptom severity, such as nasal patency measurements, smell tests and/or allergy tests.
Is there a way to measure headaches?
Headache cannot be measured in an objective way, like in blood or on scans. The location, type, severity and triggers of headache can be asked during history taking, as well as the impact of the headache on quality of life and daily functioning.
Do I need repeated CT scans to assess the extent of my nasal polyps?
Repeated CT scans are not necessary to assess the extent of the nasal polyps or to evaluate disease progress. Nasal endoscopy (looking with a camera inside the nose) remains the corner stone of follow-up and response to treatment. Only when your Ear, Nose and Throat (ENT) specialist is not sure about the extent or nature of your nasal polyps or when surgery is suggested, a CT scan is indicated.
Does a sinus CT scan cause much radiation? Are the scans necessary?
Every CT scan exposes the individual to radiation. Therefore, it is important to perform CT scans when necessary to make the correct diagnosis or to prepare a patient for sinus surgery. Your Ear, Nose and Throat (ENT) specialist will explain the indication for a CT scan. Most hospitals use a low radiation dose protocol for CT scans of the sinuses. When these protocols are used, the amount of radiation you are exposed to during each scan is equivalent to few months of exposure to natural radiation from the environment or a transatlantic flight (back and forth).
When and why is an MRI scan advised?
MRI (magnetic resonance imaging) is indicated upon specific indication in chronic rhinosinusitis. MRI is an imaging modality that does not require radiation exposure. MRI instead uses a magnetic field and radio waves to create images in the area of concern within the body. MRI is often used to evaluate disease other than chronic (rhino)sinusitis or nasal polyps, and to evaluate soft tissue disease. The MRI scan will show more details on the type and size of a lesion and its relation with surrounding soft-tissue structures. This will help your Ear, Nose and Throat (ENT) specialist in making a diagnosis and a plan of treatment.
When and why is an X-ray of the skull advised?
Ordinary X-rays (Röntgen radiation) of the skull or sinus cavities are no longer advised in patients with case of chronic (rhino)sinusitis. The interpretation of the radiologic findings on X-ray images is difficult and CT scans allow a better view on the pathology.
When should a neurologist be consulted for headache?
Headache or facial pain/pressure can be a symptom of rhinosinusitis, but also of a neurologic disorder. Headache/facial pain that comes without any other nasal symptom and without clear signs of inflammation inside the nose is rarely sinus-related and often due to neurological causes. Nausea, vomiting, aura, photophobia (discomfort or pain due to light exposure), phonophobia (discomfort or pain due to loud sounds) are symptoms that are also linked to headache that is unrelated to chronic (rhino)sinusitis and require consultation with a neurologist.
What is the second-line treatment?
The main focus in the treatment of chronic sinusitis lies on controlling the symptoms. Further treatment can also reduce the inflammation of your mucous membranes and ease the drainage of mucus from the sinuses to the nose. The first step involves rinsing the nose with salt water. In doing so, you wash out the nasal cavity and paranasal sinuses and loosen the mucus that would otherwise drip into the throat. After this procedure, nose sprays containing corticosteroids are more effective in reaching the inflamed mucous membranes.
In severe cases, a short course of corticosteroid tablets may also be prescribed in addition to a nose spray. Is your illness very severe? Then a long-term course of antibiotics may be the answer. If none of the described treatments get your symptoms under control the next step may be a sinus operation.
Functional endoscopic sinus surgery (FESS) is only recommended when other treatment methods have failed. If you suffer from severe chronic sinusitis with nasal polyps and if surgery in combination with appropriate medical treatment fails, additional therapy can be considered. A new treatment option is the use of monoclonal antibodies (also called biologics).

What is Functional endoscopic sinus surgery (FESS)?
The standard surgical procedure for rhinosinusitis is functional endoscopic sinus surgery or FESS. The goal for every patient who gets operated for chronic (rhino)sinusitis is to remove the disease in key areas, to restore adequate aeration and drainage of the sinuses, to remove nasal polyps if they are present, and overall to protect normal nasal functioning. Surgery will be suggested by your doctor when "maximal medical treatment" has failed.
Most nasal symptoms improve after sinus surgery, but the disease is often not cured. Sinus surgery is a challenging procedure and complications during surgery may occur. Recovery from sinus surgery is individual and depends on your health, your environment, and type of procedure, but most people need to recover during 2 to 3 weeks before healing of the sinus mucosa is final.
Since chronic (rhino)sinusitis is a chronic inflammatory disease surgery cannot guarantee a disease-free status after surgery. In patients in which symptoms recur, medical and surgical treatment need to be reconsidered.
What are monoclonal antibodies or biologics?
Monoclonal antibodies or biologics are designed to target specific substances in your immune system that cause inflammation. The term “biologic” is used for medications that are produced in living animals, plants, or cells, instead of through a chemical process. All of the biologic medications currently used for chronic sinusitis are antibodies, a kind of protein that occurs naturally in our bodies and plays an important role in our immune system.
Treatment with monoclonal antibodies leads to a reduction in nasal polyps, nasal congestion and the use of oral corticosteroids, together with an improvement of smell and quality of life. Monoclonal antibodies are used as an add-on option and do not always fully replace existing symptomatic treatment. This treatment tends to be expensive.
COVID-19
Is treatment with corticosteroid nasal spray recommended for patients with COVID-19 who present with loss of smell?
Presently, there is no evidence that the use of a corticosteroid nasal spray leads to an increased risk of COVID-19 infection or trigger a more severe course of COVID-19. A considerable percentage of COVID-19 patients experience loss of smell as an early sign of the disease. There is no indication that intranasal corticosteroid treatment has a positive impact on the recovery. However, there is no evidence either suggesting that this treatment has a negative impact on the symptoms and/or the development of (more severe) COVID-19. Therefore, it is recommended to continue regular treatment with your corticosteroid nasal spray for chronic rhinosinusitis.
I take tablets with corticosteroids. Should I continue my treatment during the COVID-19 pandemic?
Chronic use of tablets with corticosteroids should be avoided or used with caution in patients with chronic rhinosinusitis (CRS) during the pandemic and should only be reserved for patients with severe symptoms and in the absence of an alternative. Treatment decisions (corticosteroids, surgery or biologics) should be taken on an individual basis. In case of worsening of your CRS symptoms, contact your physician, as starting or stopping corticosteroids on yourself may induce general health risks as well as may affect your CRS control. It may also affect your susceptibility to SARS-CoV2 infection (the virus causing COVID-19).
I take biologic therapy for my chronic rhinosinusitis. Should I continue my treatment during the COVID-19 pandemic?
All patients who have tested positive for COVID-19 or show clinical signs or symptoms of COVID-19 infection, irrespective of the severity of the infection, should consult their physician to discuss continuation of their biologic therapy. Patients who have tested negative for COVID-19 or do not show clinical signs or symptoms of COVID-19 can continue the treatment, while being monitored (either face2face or remote) by their treating physician.
Treatment
Frequently Asked Questions
I don't want to take steroid tablets as I have heard there are lots of side effects. Is that true?
Oral steroid tablets are effective in reducing the degree of inflammation in rhinosinusitis, and hence very effective in reducing the symptom severity. Therefore, several patients receive oral steroids for rhinosinusitis as a measure to improve their quality of life and reduce the burden of disease. Oral steroids might have minor or major adverse effects, depending on the dosage, the duration of use, and the individual sensitivity. Long-lasting intake of tablets with steroids can influence thyroid disease, dysregulate sugar levels -particularly in patients with diabetes-, cause osteoporosis and trigger depressive or agitated feelings.
In contrast to oral steroids, nasal sprays with corticosteroids are considered safe, and rarely associated with adverse events in the body, as the uptake in the blood is minimal.
Do I need antibiotics to treat my chronic (rhino)sinusitis and for how long?
In moderate to severe symptoms of chronic (rhino)sinusitis, oral antibiotic treatment could be recommended depending on the type of rhinosinusitis, the aspect of the mucosa during examination with an endoscope, and the co-morbidities of the patient.
How does sinus surgery work?
The surgeon will insert a small tube with a tiny camera into the nostrils and guide it into the area of sinus cavities. The diseased sinus cavities are opened and the inflamed tissues will be removed using small instruments. Endoscopic surgery is usually performed as an outpatient procedure.
When is sinus surgery proposed?
Sinus surgery is being proposed when one or more of the following criteria are met:
- bothersome symptoms of rhinosinusitis despite guideline-based medical treatment
- bothersome symptoms of rhinosinusitis for which medical treatment is considered insufficient or unable to reach a good level of control
- bothersome symptoms of rhinosinusitis that are considered to respond well to surgery
What can I expect from sinus surgery?
Sinus surgery aims at the relief of most of your (rhino)sinusitis symptoms such as blocked nose, runny nose, postnasal drip (nasal secretions in the throat) and facial pain. The effects of surgery on smell impairment vary between patients and depend on the extent of the disease. Surgery is also expected to improve patient's sleep quality, work performance and daytime fatigue.
What are the risks of sinus surgery?
Sinus surgery is a challenging procedure and despite the availability of new instrumentation, minor or major complications during surgery may still occur. The major complications include bleeding, intracranial injury (inside the skull), and visual disturbances. Examples of minor complications include effusion of blood around the eye ('blue eye') or redness of the skin around the eye, watery eyes, scar formation inside the nose and persistence of the disease.
Can we predict success of sinus surgery?
Most patients do well after surgery, but up to 30% of operated patients respond insufficiently to sinus surgery, and revision surgery might be required. Negative predictors of results of surgery are the presence of asthma, aspirin intolerance, cystic fibrosis, extensive nasal polyps, smoking and occupational exposures to respiratory irritants. Data on the role of allergy on outcome of sinus surgery are contradictory.
Can sinus surgery be performed on children?
In general, we tend to be much more conservative when treating children than adults with chronic (rhino)sinusitis. Sinus surgery during childhood is preserved for really serious conditions such as persistent disease in patients with cystic fibrosis, immune deficiencies and other conditions, as well as orbital (eye) and intracranial (inside the skull) complications.
Can functional nose surgery be helpful for my sinus problems?
Surgery to improve nasal breathing, like nasal septal correction, can be helpful in specific patients with rhinosinusitis. If the septum is straight, patients might breathe better, and treatment for chronic rhinosinusitis might be more effective. If a septal deviation is fixed during the sinus surgery, this septal correction is considered to improve the result of sinus surgery.
Will surgery improve snoring and obstructive sleep apnoea?
Whether surgery will improve the symptoms of snoring and obstructive sleep apnoea depends on the amount of nasal obstruction caused by the chronic (rhino)sinusitis. As a general rule, the nose plays a small role in the problem of snoring and apnoea. Therefore, prediction of success of sinus surgery on snoring is often impossible. Your Ear, Nose and Throat (ENT) doctor can discuss the options with you.
Will medical or surgical treatment for chronic (rhino)sinusitis improve my smell?
Both medical and surgical treatment aim to reduce the inflammation in sinuses caused by (rhino)sinusitis. Nasal sprays, drops or tablets containing corticosteroids can usually clear this up and restore your sense of smell. If the medical treatment fails, sinus surgery may be considered. It is challenging to predict the degree of improvement of smell following sinus surgery, ranging from total restoration to partial or even no recuperation. Your treating physician might be able to provide you with a prediction of likelihood of success of treatment on the smell impairment.
Is sinus surgery a painful operation?
Patients experience the phase after sinus surgery as painful or not, depending on the extent of surgery, the degree of inflammation and other factors like the individual pain threshold. In case of facial pain or headache, your doctor will recommend painkillers.
How do monoclonal antibodies or biologics work?
Depending on the monoclonal antibody, they specifically target different molecules that influence your immune system mediating the disease. Some monoclonal antibodies (called anti-IgE antibodies) work by binding IgE, preventing it from binding to its receptor on the surface of inflammatory cells in your blood. IgE stands for Immunoglobulin E and is released in your blood when your immune system overreacts to an allergen. Not all monoclonal antibodies target IgE. Others target interleukins (in short: IL) or their receptor which are proteins mainly produced by white blood cells that regulate immune and inflammatory responses. Some examples are anti-IL4 and anti-IL13 antibodies who target IL-4 and IL-13. Other monoclonal antibodies target IL-5, an immune system protein that normally activates the production of a type of inflammatory cell called eosinophil.
How are monoclonal antibodies or biologics administered?
Most of the monoclonal antibodies so far on the market are administered subcutaneously (i.e. with an injection) – usually once per 2 to 4 weeks depending on the specific product. Most monoclonal antibodies are currently administered in a doctor’s office, other monoclonal antibodies can be administered at home by use of an auto-injector.
How long do I need to be treated with monoclonal antibody or biologics?
There are currently no set recommendations on how long a patient should be on a monoclonal antibody. Guidelines recommend trialling the medication for at least four months to see if it is improves your chronic sinusitis. Treatment response can be re-evaluated again after 1 year.
What are possible local side effects of treatment with monoclonal antibodies or biologics?
After injecting the monoclonal antibodies some local side effects might appear. Common local injection site effects are redness of the skin, swelling, itching and burning sensation. Severe side effects are very rare. We recommend you to discuss the possible side effects of the chosen product with your physician.
What to do after a specialist visit or surgery?
If your symptoms remain bothersome or if you develop new symptoms, it is important to take a new appointment with your doctor. In case you also experience symptoms of the lower airways such as shortness of breath, you should consider making an appointment with a pulmonologist.
In about 30% of the operated patients, symptoms still persist after surgery, and medical treatment or an operation are reconsidered. There is also less chance of surgery being successful if you have asthma, an aspirin intolerance, cystic fibrosis or large nasal polyps, or when you are exposed to irritants in your work environment.
Good follow-up is essential following the functional endoscopic sinus surgery (FESS). The surgeon deals with the affliction in your sinuses, removes any nasal polyps and restores the air flow and nasal function. Post-operative recovery takes 2 to 3 weeks and often involves nasal rinsing to loosen the mucus and blood, plus a nose spray containing corticosteroids which relieves the post-operative inflammation. During your recovery you will usually return to the surgeon, who will clear your sinuses using suction.
If you are under treatment with monoclonal antibodies or biologics, it is recommended to have regular follow-up consultations with your ENT specialist to monitor your response to treatment. If your symptoms aggravate during treatment, you should also see an ENT specialist.
Follow-up
Frequently Asked Questions
What is recommended as post-operative care after a sinus surgery?
Most sinus surgeons recommend nasal douching in combination with anti-inflammatory nasal or oral treatment in the postoperative phase. Nasal douching helps to evacuate secretions and blood during the postoperative phase, whereas anti-inflammatory treatment like corticosteroids reduce the post-operative inflammation. This post-operative treatment regimen is often combined with regular visits to the surgeons, allowing suction cleanings of the sinonasal cavities.
Why do my symptoms recur after surgery?
It has been reported in scientific papers that in approximately 20% of patients undergoing surgery, symptoms will recur due to recurrent inflammation. Patients with asthma, sinusitis where the upper (frontal) sinuses are affected or with thickening of the bones of the sinus cavities, with aspirin-exacerbated respiratory disease (AERD) and with exposure to occupational agents have been connected with poorer surgical outcomes. The extent of inflammation and bleeding during surgery, the surgical skills, the extent of surgery also affect the outcomes. Post-operative care is just as critical as pre-operative assessment and techniques used during surgery. Patients must be prepared to meticulously rinse the nasal cavity with saline solutions and use nasal corticosteroid sprays.
Why do nasal polyps grow back?
Chronic (rhino)sinusitis with nasal polyps is a chronic disease of the sinonasal mucosa with grapelike structures (called polyps) causing symptoms. Polyps are mucosal structures with chronic inflammation being responsible for the volume and the persistence. Therefore, anti-inflammatory treatment with corticosteroids and douching with saline are recommended.
My polyps were operated, and they did not come back. Why do I still not smell properly?
Smell loss is one of the cardinal symptoms of rhinosinusitis with nasal polyps, either caused by obstruction of the smell organ (olfactory organ) by the polyps, or by inflammation of mucosa of the smell organ. Despite removal of nasal polyps by surgery, inflammation in the olfactory region might persist. As a consequence, not all patients experience a normal smell capacity after sinus surgery. It may therefore be important to apply nasal sprays containing corticosteroids after surgery because they reduce the inflammation of the olfactory (smell) mucosa.
Galenus Health App
Download the App for free
Together we aim for less complaints, so you can start enjoying life today